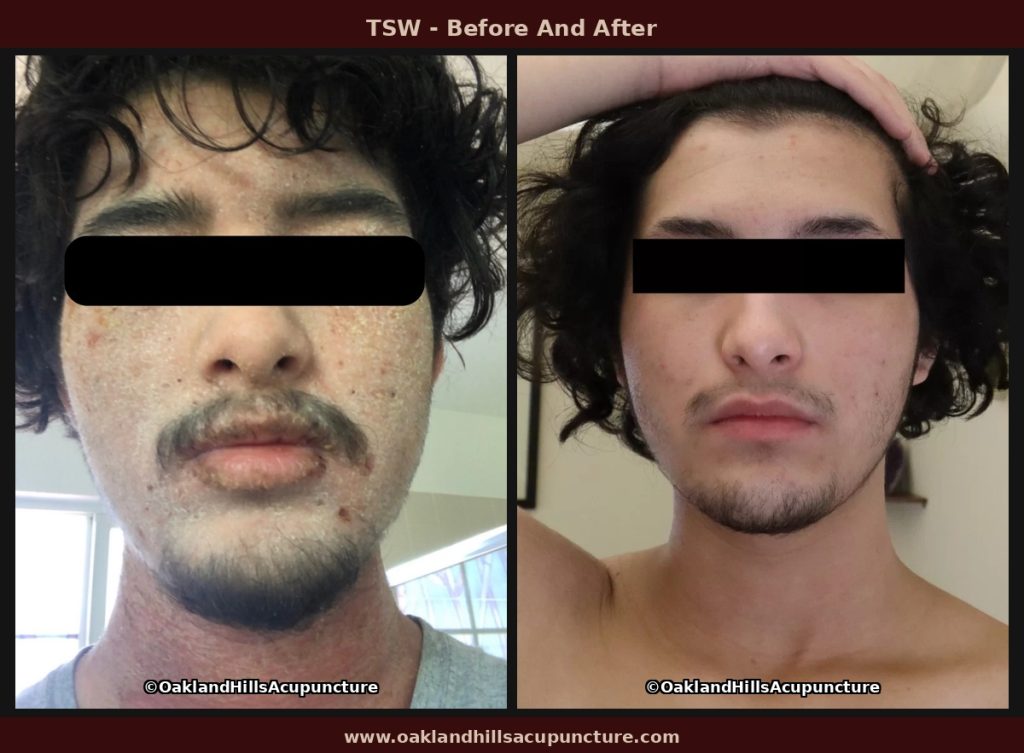
In my previous post, I walked through the four stages of topical steroid withdrawal, the hallmark clinical signs, and how to distinguish TSW from an eczema flare. Understanding what is happening to the skin is a necessary first step. The next question most patients ask is: what can actually be done about it?
This post explains how Chinese herbal medicine addresses TSW — what the treatment looks like in practice, how formulas are individualized and adjusted over time, what kind of improvements are realistic, and what the emerging research says about why this approach may work.
Why Chinese Herbal Medicine for TSW?
Topical steroid withdrawal, by definition, is a condition created by a medication. The skin’s immune activity has been artificially suppressed by steroid use, and when that suppression is removed, the resulting inflammatory rebound can be severe. The challenge for any treatment approach is to support the skin’s recovery without reintroducing the kind of suppression that caused the problem in the first place.
Chinese herbal medicine addresses this in a fundamentally different way than most conventional options. Rather than targeting a single inflammatory pathway or suppressing the immune response broadly, herbal formulas work through multiple mechanisms simultaneously — reducing inflammation, supporting the skin barrier, improving circulation to damaged tissue, and addressing systemic issues like disrupted sleep and temperature regulation that accompany TSW.
The formulas are individualized. Two patients with TSW may present very differently — one with intense burning and widespread redness, another with heavy oozing and crusting — and they will receive different herbal prescriptions. This is not a one-size-fits-all approach, and that individualization is a meaningful part of why it works.
How Treatment Works in Practice
My primary treatment for TSW is individualized oral Chinese herbal formulas, prescribed as concentrated granular extracts. Patients dissolve the granules in hot water and drink the formula two to three times daily. The formula is tailored to the specific presentation at each visit and modified as the condition evolves.
The Diagnostic Process
The diagnostic process and first visit should start at minimum two weeks after the last usage of topical steroids.
Before prescribing, I conduct a detailed assessment that goes well beyond looking at the skin. Chinese medicine diagnosis involves evaluating the skin’s appearance — the color, texture, moisture, heat, and distribution of lesions — alongside a range of systemic questions. I ask about body temperature fluctuations, thirst, digestion, energy, sleep quality, the nature and timing of itch, emotional state, and menstrual health where relevant.
One important distinction to make is what condition the patient had before developing TSW. The majority would have suffered atopic eczema, however not all. TSW can also result from the overuse of steroids in other conditions such as lichen planus, psoriasis, pityriasis rubra pilaris, and seborrheic dermatitis, to name a few.
The information gathered in the exam and interview is used to identify the underlying patterns driving the condition. In Chinese medicine, TSW can present with very different internal patterns from one patient to the next. One patient may present with a pattern dominated by intense heat and inflammation. Another may show more dampness — oozing, swelling, and edema. A third may present with pronounced dryness and depletion. Most TSW patients actually present with a combination of patterns, and the specific ratio determines the formula.
An important point in practice is not to rigidly pair specific Chinese medicine patterns with the specific TSW stages that have started to be developed and which were reviewed in the first post. I find that many patients present with significant overlap between these “stages,” patients cycle between them, and the Chinese medicine diagnosis needs to reflect what is actually happening in front of me and the trajectory the patient appears to be on — not what a staging model predicts should be happening. Every visit is a fresh assessment.
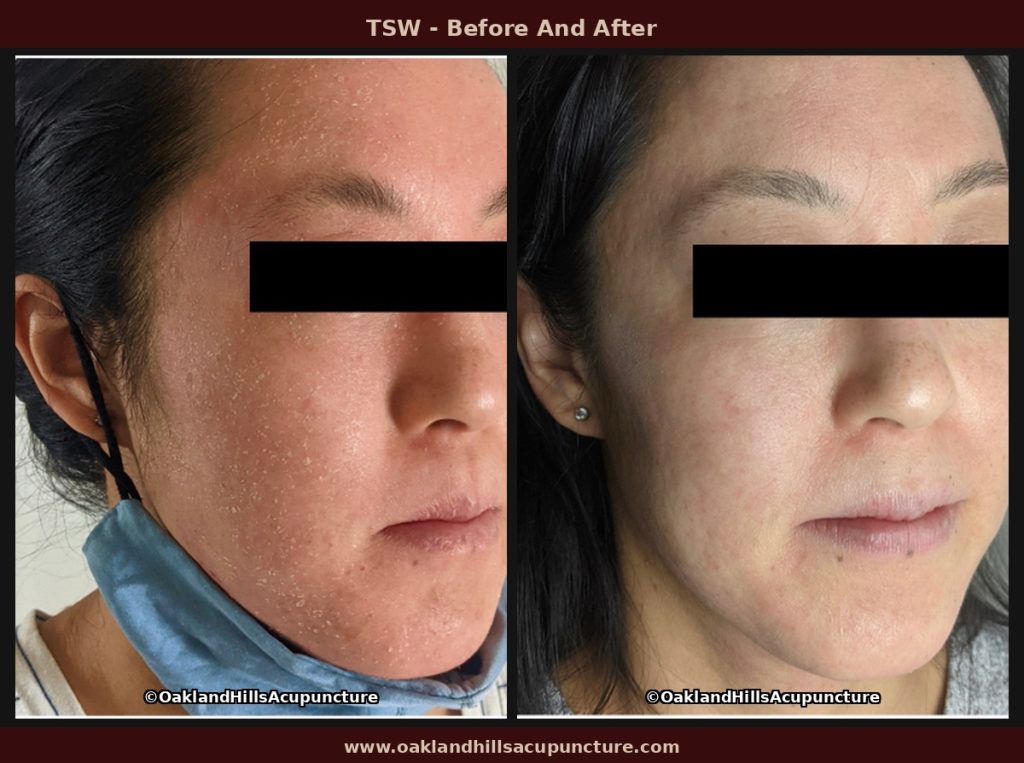
Three Phases of Treatment
While every case is different, treatment generally moves through three very broad phases. The boundaries between them are not always distinct, and the pace depends on the individual. Whatever “stage” the patient presents in, in order to move them out of the cycle of repeated flare-ups, treatment goes through these three phases.
Phase 1 — Clearing. In the acute phase, the priority in TCM terms is to clear heat, resolve toxicity, and reduce the intensity of the inflammatory response. In layman’s terms, this phase involves clearing the body of the toxic and inflammatory compounds that have built up and are driving the disease in a more severe direction. As these pathogenic compounds are cleared, several symptoms of their presence begin to resolve. Typically in this phase of treatment, we start to see a reduction — or in some cases resolution — of severe heat, heat at night, insomnia, severe scaling and desquamation of the skin (waking up with skin flakes covering the bed), edema or swelling of the face or other areas, itch attacks (random or at certain times), oozing, crusting, and more. The herbal formulas in this phase tend to be cooling and bitter — and I will be honest, they do not always taste good, but they are excellent for resolving the most inflammatory processes behind TSW and eczema. In regards to taste, most patients adjust within the first week or two, and the motivation of seeing their skin begin to respond helps. Patients often notice improvements in heat sensation, burning, oozing, and sleep within the first two to four weeks.
Phase 2 — Harmonizing. As the acute heat and oozing subside, the formula gradually shifts. The cooling herbs are reduced and the formula gradually begins to incorporate ingredients that address dryness, support the skin’s recovery, and begin working on post-inflammatory hyperpigmentation. This is a transitional phase where the balance of the formula matters — moving too quickly toward moistening while residual heat remains will not produce results. The cycle of flaring up, followed by some resolution, then flaring up again should have started to improve by this point. However, flare-ups do not always stop outright right away. In this intermediary phase, flare-ups can often still occur but with either reduced intensity and/or reduced frequency as we move out of the tendency for massive flares. Therefore it is important to take the time, be patient, and adjust the balance of the formulas visit by visit. This is one of the more nuanced aspects of treatment.
Phase 3 — Consolidation. Once the skin has substantially cleared, a lighter formula supports the body’s constitution and aims to prevent relapse. This phase is important for long-term stability. I encourage patients not to skip it — the temptation to stop treatment once the skin looks better is understandable, but premature discontinuation increases the risk of flare.
What the Herbal Formulas Actually Contain
Chinese herbal formulas for TSW typically include anywhere from eight to sixteen or so individual herbs, combined in specific proportions. The herbs are not chosen randomly — each one has documented pharmacological properties, and they are combined based on centuries of clinical use refined by modern understanding.
Without getting into specific formulas (since every patient’s formula is different), the categories of herbs commonly used in TSW treatment include:
•Heat-clearing herbs: These have demonstrated anti-inflammatory and antimicrobial properties. They form the backbone of treatment in the acute phase, helping to reduce the widespread erythema and burning that characterize early TSW.
•Blood-cooling herbs: Address deep redness and the sensation of heat radiating from the skin. In pharmacological terms, these herbs address many of the prime inflammatory drivers of TSW, and many of them modulate vascular inflammation and reduce capillary permeability.
•Dampness-resolving herbs: Used when oozing, crusting, or swelling is prominent. These herbs help dry excessive exudate and reduce edema.
•Wind-dispelling herbs: Address itch, scaling, and lichenification, which in Chinese medicine is often attributed to “wind.” Many of these herbs have demonstrated anti-pruritic and anti-inflammatory activity, with some showing effects on histamine-mediated itch pathways. In Chinese medicine, these herbs have a tendency to help regulate abnormal functioning at the body’s exterior — sometimes referred to as the Wei level from the viewpoint of the Wen Bing (Warm Disease) School of thought. Research on Chinese herbal medicine more broadly finds that many of these compounds help support epidermal barrier function.
•Fluid and Yin-nourishing and moistening herbs: Introduced more prominently as the acute phase subsides and dryness becomes the dominant feature. These support the skin barrier and tissue repair.
•Qi and blood tonics: Support overall recovery, energy, and immune regulation, particularly in the consolidation phase.
The specific combination shifts as the patient’s condition changes. A formula written in week one will look meaningfully different from the formula at month three. This adaptability is one of the key advantages of the approach.
How These Herbs Work at the Immune Level
Both TSW and eczema involve measurable dysregulation of specific immune pathways. In atopic dermatitis, the immune response is skewed toward a Th2-dominant profile, with overexpression of cytokines including IL-4, IL-13, IL-22, and TNF-α. IL-4 and IL-13 drive type 2 inflammation and directly impair the skin barrier by downregulating structural proteins like filaggrin and claudin-1. IL-22 contributes to epidermal thickening and further barrier disruption. TNF-α amplifies the overall inflammatory cascade. In TSW specifically, prolonged steroid use upregulates thymic stromal lymphopoietin (TSLP), which further shifts the immune system toward this Th2-dominant state, while mitochondrial dysfunction leads to excess NAD+ and a distinct neuroinflammatory component.
What is increasingly well documented is that many of the herbs used in Chinese medicine dermatology formulas directly modulate these same pathways. Berberine, found in Huang Lian (Coptis) and Huang Bai (Phellodendron), both commonly used in TSW formulas, has been shown to downregulate TNF-α, IL-1β, IL-6, and MCP-1, and to inhibit the NF-κB and JAK/STAT3 signaling pathways that drive inflammatory gene expression. Baicalein, derived from Huang Qin (Scutellaria), reduces serum levels of TNF-α and IL-6 and has demonstrated the ability to decrease immune cell infiltration in dermatitis models. Paeoniflorin, from Bai Shao (White Peony), helps rebalance the Th1/Th2 ratio and has been shown to suppress NLRP3 inflammasome activation and regulate IgE production.
This is not a case of traditional medicine operating separately from modern pharmacology, the mechanisms overlap significantly. The difference is that a Chinese herbal formula combines multiple compounds targeting multiple pathways simultaneously, rather than isolating a single target the way most pharmaceuticals do. Importantly, these herbs function as immunomodulators rather than immunosuppressors. Where corticosteroids and some biologics work by broadly suppressing immune activity, compounds like paeoniflorin have demonstrated bidirectional immune regulation — simultaneously suppressing overactive pro-inflammatory (M1) macrophage responses while enhancing anti-inflammatory (M2) activity, effectively rebalancing the immune system rather than shutting it down. This multi-target, immunoregulatory approach may help explain why herbal treatment can address the broad, systemic nature of TSW — the skin inflammation, the immune dysregulation, the sleep disruption, and the temperature instability — in a way that single-pathway interventions often cannot.
What the Research Shows
Research on Chinese herbal medicine specifically for TSW is still emerging, but the existing evidence is encouraging and growing.
A 2025 case series published in the Journal of Integrative Dermatology documented five adult TSW patients treated with individualized Chinese herbal medicine. All five patients showed resolution of thermodysregulation and sleep disturbances, and two of the five achieved complete resolution of all five tracked acute symptoms — erythroderma, thermodysregulation, oozing, itch and pain, and sleep disturbances. Treatment durations ranged from three to thirteen months.
A separate case report published in Allergy, Asthma, and Clinical Immunology described a seven-year-old boy with severe eczema complicated by corticosteroid withdrawal syndrome. After seventeen months of multicomponent Chinese herbal medicine (oral herbs, herbal bath, and topical herbal cream), the patient showed marked improvement in skin lesions, sleep, and itch — and did not require any oral or topical steroids during the entire treatment period. His serum IgE decreased by 75% and eosinophil counts decreased by 60%.
On the broader evidence for Chinese herbal medicine in inflammatory skin disease, a 2022 systematic review of eight high-quality randomized placebo-controlled trials in atopic dermatitis found that Chinese herbal medicine significantly improved skin lesion severity (as measured by EASI-90, SCORAD, and body surface area scores) and sleep quality compared to placebo.
There is also a noteworthy convergence between Chinese medicine and Western research. The 2025 NIAID pilot study that identified elevated NAD+ levels as a biomarker of TSW also found that berberine — a compound that has been used in Chinese herbal medicine for centuries (it is found in herbs like Huang Lian and Huang Bai, both commonly used in TSW formulas) — improved TSW symptoms through inhibition of mitochondrial complex I. A follow-up case series of sixteen patients published in the Journal of Clinical Medicine in 2026 reported that patients using berberine showed smoother skin, less erythema, and decreased flaking. This is a remarkable instance of modern research validating a traditional treatment approach at the molecular level.
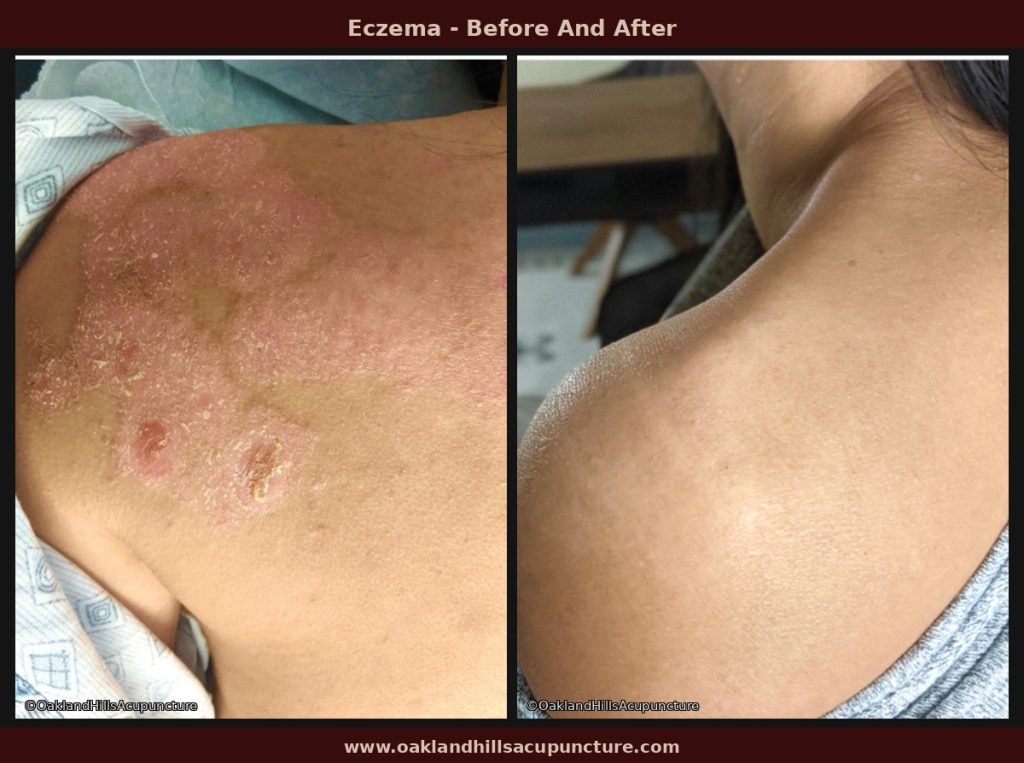
What to Expect: A Realistic Timeline
Setting honest expectations is important. TSW is a complex condition, and while Chinese herbal medicine can significantly support the recovery process, it is not an overnight solution. The following reflects a general pattern of improvement for patients who follow their herbal plan consistently, though individual timelines vary:
•Weeks 2–4: Improvements in heat sensation, nighttime burning, and sleep. Many patients notice the intensity of the burning begin to diminish. Oozing, when present, typically begins to decrease.
•Months 1–3: Significant reduction in redness, flaking, and oozing. Flares become less frequent and less intense. The skin begins to stabilize and clear.
•Months 3–6: Continued clearing with the skin approaching a stable state. Post-inflammatory hyperpigmentation begins to fade. Some patients may complete treatment by six months, including consolidation.
•Months 5–12: Consolidation and ongoing support. The overall treatment course for most TSW cases falls within this range. Some patients still need treatment to address trouble spots with persistent symptoms.
Initial visits are typically every two weeks, gradually extending to three weeks as the skin stabilizes. In the consolidation phase, visits may be monthly. Compliance with the herbal formula is important — the herbs work best when taken consistently as directed.
I should also note what herbal medicine cannot do. It cannot reverse symptoms overnight, it cannot reliably prevent all symptoms of a rebound after stopping steroids, and it will not eliminate all discomfort in the early stages of treatment. What it can do — and what I see consistently in practice — is meaningfully reduce the severity and duration of TSW, improve quality of life during the recovery process, and support a more stable long-term outcome.
What Makes This Approach Different
Patients often ask how Chinese herbal medicine compares to other treatment options they have considered. A few key distinctions:
•Individualization: The formula is specific to you and adjusted at every visit. It is not a fixed protocol or a single supplement.
•Non-steroidal: The herbs do not suppress the skin in the way that topical steroids do. The goal is to support the skin’s own recovery, not to replace one form of suppression with another. Neither the oral herbs nor any topical herb ointments or baths for infants contain corticosteroids.
•Whole-person treatment: The formula addresses not only the skin but also sleep, digestion, energy, and temperature regulation — all of which are commonly disrupted in TSW.
•Adaptability: As the condition evolves, the formula evolves with it. This responsiveness is difficult to achieve with fixed-dose pharmaceuticals.
What This Means for You
If you are navigating topical steroid withdrawal and wondering whether Chinese herbal medicine might help, the short answer is: in my clinical experience, it can — significantly. The treatment is not simple, the herbs are not always pleasant, and the process requires patience and consistency. But for patients who commit to the process, the results I have seen are more than encouraging.
I see my role as supporting patients who have already made the decision to discontinue topical steroids. I do not push patients toward stopping — that is a personal decision. But once that decision is made, I believe Chinese herbal medicine is one of the most effective tools available for managing what comes next.
In my next post, I will discuss the realistic timeline for TSW recovery in more detail — what the research says about how long recovery takes, what factors influence the timeline, and how to think about progress when improvement feels slow.
David Heron, DACM, L.Ac. is a Chinese medicine dermatology specialist at Oakland Hills Acupuncture in Oakland, CA. He treats TSW, eczema, and other complex skin conditions in person, serving patients throughout the East Bay — including Oakland, Berkeley, Alameda, San Leandro, Walnut Creek, Orinda, Lafayette, Piedmont, and Emeryville — and accepts select patients in California via telemedicine.
To schedule an appointment, visit oaklandhillsacupuncture.com/schedule or call the clinic directly.
